Find Reliable Relief from Dry Eye at Visionarium Optometry
That scratchy, gritty feeling in your eyes? The watery irritation that just won’t seem to go away, especially after a long day spent working at a computer? You could be experiencing dry eye disease. At Visionarium Optometry, we know how disruptive dry eye symptoms can be, and that’s why we’re here to help.
Dry eye is a chronic condition, but by pinpointing its root cause with diagnostic technology like LipiView, we can create a tailored treatment plan to restore your comfort.
Our dry eye solutions include proven treatment options such as OptiLIGHT IPL, LipiFlow, and TearCare, alongside other effective therapies, to bring you lasting relief. Don’t settle for temporary solutions when long-term dry eye care is available to you.

Dry Eye Diagnosis at Visionarium Optometry
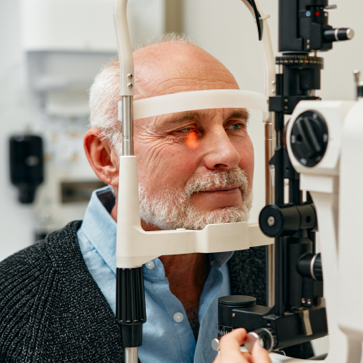
At Visionarium, diagnosing your dry eye is the first step to planning effective treatment. Using LipiView, we can assess the quality of your tear film, the health of your meibomian glands, and test your blink dynamics. This key testing helps us determine the exact cause of your dry eye symptoms and craft a solution tailored specifically for you.
When you visit us for a dry eye evaluation, we will:
- Ask about your symptoms, daily activities, and medical history
- Use LipiView to evaluate how much oil (meibum) is present in your tears
- Capture close-up photos of the meibomian glands along your eyelids to see how many of them are damaged or even completely non-functional
- Check your blink dynamics to see if your blinks are properly dispersing protective tears across your eyes’ surfaces
- Evaluate external contributing factors such as screen time or exposure to dry environments

What Is Dry Eye Disease?
Dry eye happens when your tear film is out of balance, typically for 1 of 2 reasons:
- Evaporative Dry Eye: This is most commonly caused by meibomian gland dysfunction (MGD), where essential oil-producing glands in your eyelids are blocked or compromised. Without a healthy oil (lipid) layer, tears evaporate too quickly.
- Aqueous-Deficient Dry Eye: When there’s insufficient tear production, leaving your eyes under-lubricated.
Symptoms of dry eye can include redness, irritation, a gritty feeling, watery eyes, or even blurry vision. Factors such as extended screen time, windy or smoky conditions, certain medications, and blepharitis can exacerbate your symptoms.
Dry Eye Quiz

Personalized Dry Eye Treatments for Long-Lasting Relief
After identifying the root cause of your dry eye, we’ll create a customized care plan for you—because no 2 cases are the same. Our goal is to create a plan that works for your life, is easy to incorporate into your routine, and provides lasting relief.
Here’s an overview of the innovative dry eye therapies and tools we may recommend.
BlephEx is a short, in-office treatment that gently removes debris and bacteria from your eyelids, reducing inflammation caused by blepharitis.
LipiFlow is a gentle, in-office treatment designed to unclog and restore function to your meibomian glands, a common cause of dry eye. By improving gland function and enhancing tear quality, it helps provide lasting relief and protect your eye health.
A clinical study found 79% of patients reported noticeable improvement in their dry eye symptoms within 4 weeks of a single LipiFlow treatment.
There’s no downtime or recovery period after your procedure. Most patients notice improvement within 4 to 8 weeks as their ocular surfaces return to normal. Another study showed that 90% of patients had significant symptom relief (a 50% improvement) by their 8-week follow-up. It has also been shown that further improvement can be seen at 6 months.
Although we always hope everyone will see improvement, some patients with severe disease may not. For severe dry eye disease, the goal of treatment is to halt its progression.
TearCare uses targeted, gentle heat to melt blockages in the meibomian glands, a key contributor to dry eye. By restoring natural gland function and enhancing tear quality, it offers effective, lasting relief while supporting overall eye health.
TearCare can improve the quality of your tears and reduce symptoms like dryness, gritty or scratchy sensations, blurry vision, and watery eyes.
OptiLIGHT is FDA-approved intense pulsed light therapy that reduces inflammation, strengthens the tear film, and curbs bacteria and Demodex mites.
OptiLIGHT IPL can significantly relieve dry eye indicators. Typically, we recommend multiple treatments over several weeks to achieve the full effect.
OptiLIFT uses Dynamic Muscle Stimulation (DMSt) to activate muscle contractions around the lower eyes. This helps to restore function to weakened periorbital muscles and improve blinking.
OptiLIFT can reduce dryness due to poor or incomplete blinking. It also enhances muscle tone and tightness around the eyes, resulting in a lifted, more youthful appearance.
Specially formulated eyelid sprays are designed to cleanse and hydrate the eyelids, reducing inflammation and irritation associated with dry eye. They help maintain eyelid hygiene and improve overall eye comfort.
Your Visionarium optometrist may prescribe medicated eye drops to reduce inflammation or stimulate tear production, providing targeted relief for moderate to severe dry eye symptoms.
Nutritional supplements can support your eye health by enhancing the quality of tears and reducing inflammation associated with dryness. These are often recommended as a natural way to ease dry eye discomfort.
Warm compress masks deliver soothing heat to the eyelids, helping to loosen blockages in the meibomian glands that can cause dry eye. They can enhance tear quality and offer relief from dryness and irritation.

Why Choose Visionarium Optometry for Dry Eye Treatment?
We’re dedicated to bringing you relief from dry eye symptoms, so you can get through your day without thinking about how your eyes feel. Trust our team, tools, and knowledge to treat your symptoms.
From in-office treatments to at-home solutions, we offer a holistic approach tailored to your needs. Our team is here to address your concerns and keep you informed throughout the entire process.
Let us help you find relief and take back control of your eye health.

In-Depth Dry Eye Treatment
Are dry, irritated eyes interfering with your life? Our thorough diagnostic approach is designed to identify the source of your tear film imbalance, allowing us to create a personalized plan that brings you relief and protects your vision.
From lid imaging and tear evaluation to heat-based and energy-based dry eye treatments, we’re here to help you see and feel better.


Our Google Reviews
Testimonials
“Doctor Quan and the whole staff are great and very helpful. When I needed to see him in an emergency, he squeezed me in between other patients.”
George P.
“Doctor Quan and the whole staff are great and very helpful. When I needed to see him in an emergency, he squeezed me in between other patients.”
George P.
Visit Our Eye Clinic
Find Us
We’re in Lakeshore Plaza near Ross Dress for Less,
just off Sloat Boulevard, in the Outer Sunset.
Where to Park
There’s plenty of free parking in our lot at Lakeshore Plaza.
Our Address
- 1551 Sloat Blvd
- San Francisco, CA 94132
Contact
Information
Hours of Operation







Protect Your Nearsighted Child’s Vision with Myopia Control
If your child is nearsighted, regular glasses often aren’t enough. We can do more to protect their vision thanks to myopia control!
A nearsighted child can’t clearly see distant objects, and their sight tends to worsen as they grow. Typically, this worsening vision is due to their eyes growing longer than necessary, which raises the risk of certain eye diseases in the future.
With myopia control, we can prescribe specialized contact lenses that can correct their vision and slow the unwanted elongation of their eyes. We can also prescribe uniquely formulated eyedrops to slow the elongation of the eyes.